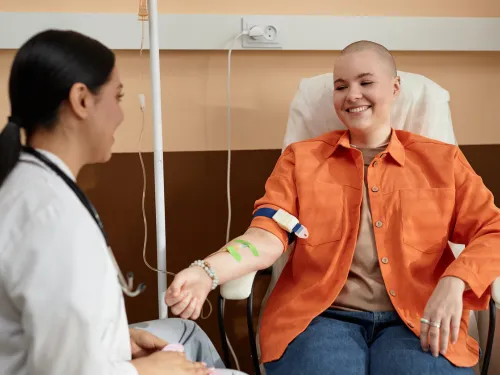In October 2021, a scan found a cyst on my ovary. Despite being told it was big for my height and build, I was advised that cysts are quite common and often resolve themselves, and therefore no action was going to be taken.
I carried on with my life, but around a year later, I started developing signs and symptoms that I wasn’t sure what to put down to. I booked an appointment at my GP’s, where I thought I’d tell them about my problems and then hopefully, they’d be able to help me.
My stomach had become increasingly bloated, and I had this hard lump on my lower abdomen which was more prominent in the morning and wasn’t going away. I explained this at my appointment but was advised that this was most likely irritable bowel syndrome (IBS). About three weeks later, though, I went back and told them that the lump was now constant, not just more prominent in the morning, and it looked to be growing. I told them about the other symptoms I was having, like constantly going to the toilet yet not emptying fully. I was also always hungry, but as soon as I had just one mouthful of food, I’d feel full. I was also suffering from fatigue and back pain, symptoms I now know to be associated with ovarian cancer. I also mentioned to them about a history of cancer in women in my family, which wasn’t listened to. Instead, I was again told that I most likely had IBS, but they’d send me for scans to be sure.
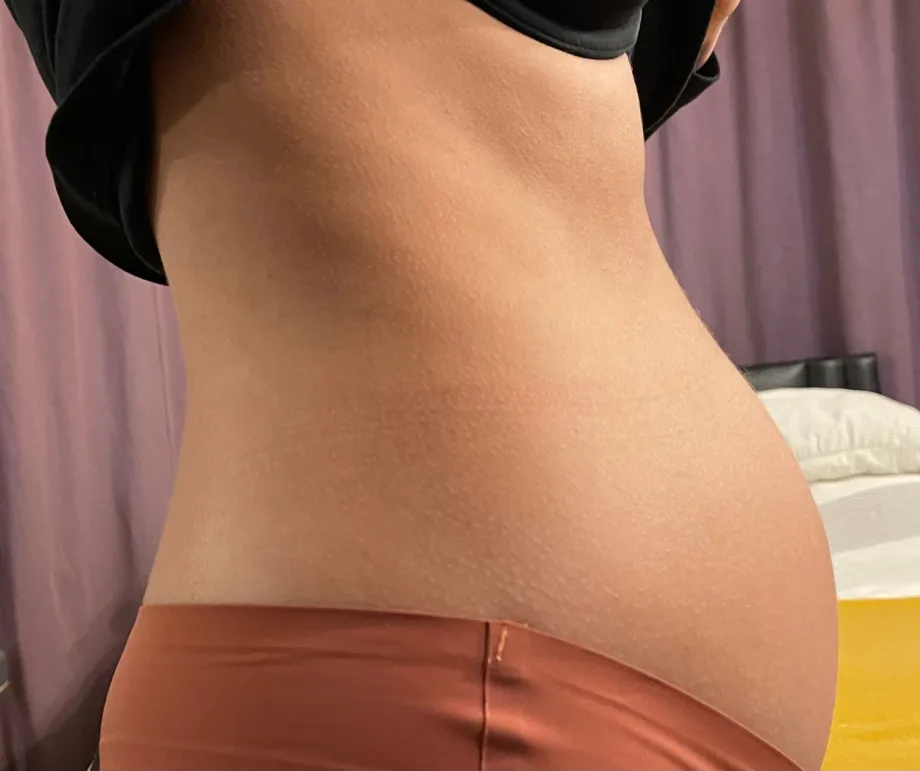
Less than a week later, I contacted them again as, by then, I was really worried. This time I was taken more seriously and was sent for emergency scans. I had the scans and the radiographer wasn’t happy with what she could see and sent me straight to majors. At this point, I thought this was a good thing, as it meant something was finally being done, but I was also alone and scared of what might come.
After a further scan, the doctor quickly referred me to the cancer clinic. She told me not to worry as it was unlikely to be cancer, but it was a precautionary measure, after having mentioned my family history of cancer in women to her. When I got there, I was told that specialists had looked at the cyst and didn’t think it looked cancerous. However, as it had grown so much, it would require surgery, cutting me down the abdomen. By this point, I looked like I was about to give birth, so although anxious, I was glad something was being done.
Diagnosis and further treatment
My surgery had some complications, but the cyst, which held just under two litres of fluid, was removed. After the operation, I was told that I’d hear back within four weeks if something was wrong, and if not, I’d just have a check-up to see if everything was okay and then I’d be able to move on. Eleven days later, however, I received a call from the hospital asking me to come in. This sent me into a panic, and I knew straight away that something wasn’t right.
When I got to the hospital, I was told that the cyst was cancerous, and I’d have to undergo another surgery to remove my ovary, fallopian tube, omentum and appendix. The surgery went well but by this time, I was really feeling what I’d been through. In under six weeks, I’d been told I had a rare form of cancer, which affects just 200 people in the UK each year, and had two major surgeries to get rid of it. To say there’d been a lot going on was an understatement.
I thought that was it but was advised that due to complications from my first surgery, there was a risk that the cancer cells may have spread. Because of this they wanted to do six rounds of intensive chemotherapy, even though chemotherapy wasn’t standard for my cancer type. It just felt like one thing after another, and before chemo even began, I also had to undergo fertility treatment as I only had one ovary, and the chemotherapy could leave me infertile. This felt like another thing stacked onto me. It was already a lot to take in, but there I was, just 22, and having to think of my fertility.
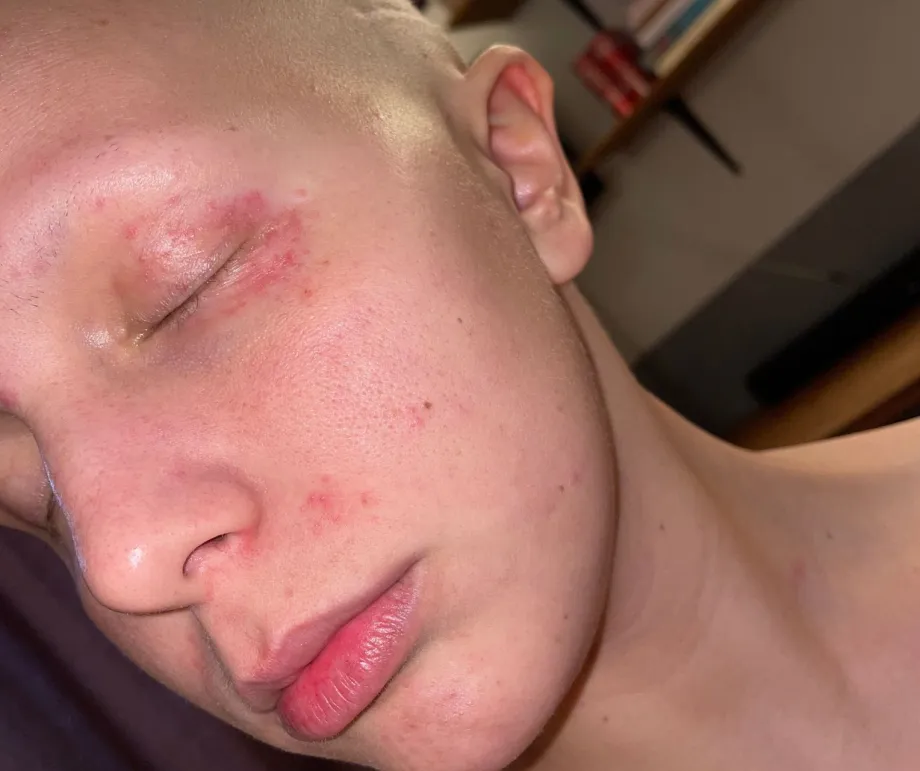
Finishing treatment and the long-term impact of cancer
I think a common misconception amongst the general public is that everything is better once treatment for cancer finishes, but it doesn’t work like that. When I finished my chemo, it left me feeling a little vulnerable. I’d had the all-clear, and that was obviously great, but I was now on my own. I’d gotten used to having the support of my medical team and had used to placing my trust in them to look after me. And then, it was finished and I was expected to just get on with life. People would say to me, ‘Yeah, but it’s over with’, not realising how much there still is to deal with, even to this day. To process and unpack. To get used to living with.
I’d finished treatment, but I had to find myself. To rebuild. But that hasn’t been easy. I don't have the energy that I once did. I have long-term side effects including problems with my hearing and neuropathy. I'm constantly going to the doctors because I’ve got no immune system. My joints and muscles are always aching. I have memory loss. I can be having a conversation with someone and then completely lose my train of thought. I'm a lot more tired and it isn't a tiredness that can be fixed by sleep, it's a constant tiredness.
Now, my life is dictated by hospital appointments, and I’m not able to do a full-time job. There's a lot to it that I don’t think people understand. Even now, I'm still trying to be patient with myself and just be proud of where I am and how far I’ve come. When I’m down, I find it really frustrating for people to still say, ‘You’re here, just get over it’, without comprehending just how much I’ve been through – and am still going through.
I don’t think people see the aftermath of cancer treatment. Life happens, but for survivors, we’ve still got appointments and check-ups, which we'll be having for the rest of our lives. The side effects are both physical and mental, with so much to
unpack. There shouldn’t be a timeline on how long a young person should take to process what’s happened to them.
Yes, we’re not on active treatment, but people don’t see the scans (and the anxiety around scans), the blood tests, the phone calls, or the constant appointments. More awareness is needed on this, to help people understand what it’s like, and I hope that by sharing my story it will help these conversations feel a little less taboo.

Why I share my story
The whole cancer experience, especially for a young person, is a very isolating experience. It feels very lonely. After my diagnosis, I shut everyone off and hardly told anyone about it. I didn’t want to see or talk to anyone. It was very much an identity crisis, and I just felt so alone. I thought nobody's going to understand me because they weren’t going through it. Something changed when I started an Instagram account to document my experiences, the accompanying challenges, and what helped me. By doing this, I connected with so many other people going through similar things to me. People who I’ve been able to joke with about what we’ve both been through or help each other with advice and support.
At first, I didn’t want to listen to other people’s stories, I couldn't see how it would help me. Now, I’m glad I did, as it’s helped me feel less alone in what I’ve been feeling. It’s lightened the load a bit, and I hope that by sharing mine, it has for others, too.
My message to people worried about their health
One thing I’m really passionate about, is advocating for people to be seen. I hope that by sharing my story, it helps them advocate for themselves. If you’re worried about signs and symptoms, it’s important that you don’t just speak up, but persevere until you're taken seriously. Trust your instincts when something doesn’t feel right.

How can people support a young person with cancer?
When it comes to supporting a young person with cancer, don’t wait to be asked for something. Don’t say to someone with cancer, “message me” or “call me when you need me”. They don’t have the time or energy to be thinking of how you can help, so just do it. They won’t mind if you go round or prepare a meal for them, they’ll be grateful. So, take on that responsibility to treat them.
I’d also say to treat them as the person that you've always known them to be. They are still who they are. Yes, they’ve got a cancer diagnosis, but treating them any differently because of it, will only make an isolating time feel even more so. Have the kindness to acknowledge it’s happening and, yes, it's bad, but don’t make it their whole personality. They’re still human at the end of the day. Treat them with kindness.